Advancing Disability-Inclusive Healthcare (ADIH)
Empowering health professionals to provide exceptional care for individuals with disabilities through a curriculum for lifelong learning.
Advancing Disability-Inclusive Healthcare (ADIH)
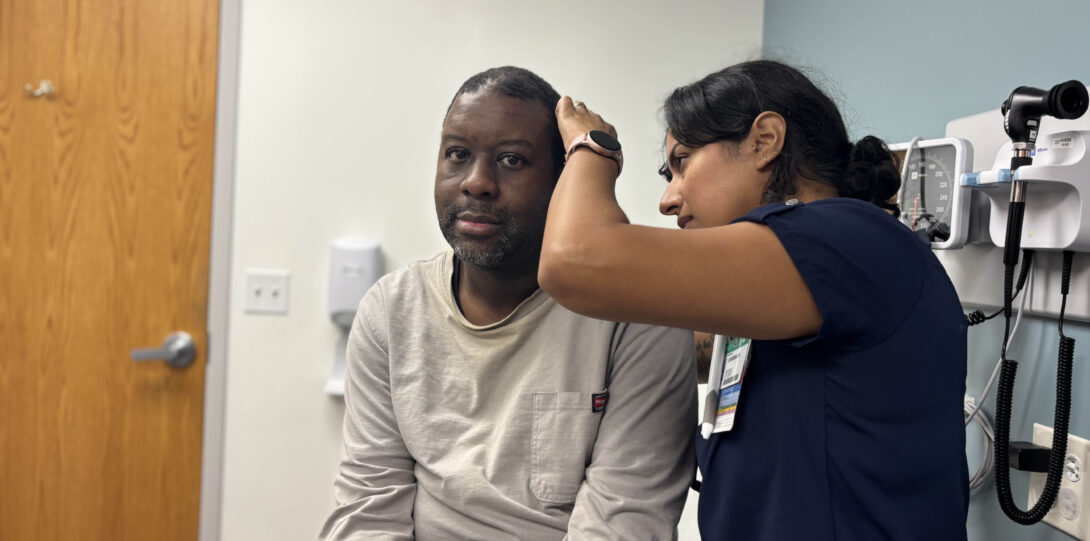
It is no secret that healthcare has not served the needs of people with disabilities well. Despite repeated calls to teach healthcare professionals a comprehensive model of holistic care, centering the perspectives of people with disabilities, little has changed. Why? We believe many healthcare training programs do recognize and desire to change but simply do not have the curricular tools and resources. We hope that this website helps to close this gap.
The guiding principles we have used in building the curricula are:
- Grounding disability in a holistic biopsychosocial model.
- Centering the perspectives of people with disabilities as the experts in their conditions.
- Adopting inclusive and universal learning strategies.
- Integrating high-quality materials that have been developed by others.
© 2025 The Board of Trustees of the University of Illinois. All rights reserved.

It’s such a valuable undertaking to help medical professionals see disability from the perspective of individuals with disabilities ourselves. It’s helpful and crucial I believe for physicians and others to see that those with functional limitations are not perennial patients. Yes, from time to time we have needs and health concerns that require the expertise of those in the healthcare field, we also have dreams and heartaches and responsibilities and joys that may have very little to do with a diagnosis, functional limitation or impairment.
| Children's Author, Educator and Advocator
Genesis of the ADIH project at UIC
The genesis of and commitment to ADIH at the University of Illinois Chicago (UIC) began in 2019. Three seasoned clinicians, from disparate backgrounds (Kirschner, Keehn, & Caskey), began to have conversations about the barriers people with disabilities (PWD) face in the healthcare system. These included:
- Lack of accessible, disability-competent clinical services.
- Lack of training in health professions programs about disability as a complex biopsychosocial phenomenon.
- Lack of adequate social supports, including home and community-based services and funding to support the sustainability of the clinical care services.
UIC ADIH Steering Committee

“Our mission is rooted in providing equitable, compassionate, and inclusive care to all, especially those who are most vulnerable. Providing comprehensive care for individuals with disabilities is central to this mission.”
Rachel Caskey | MD , MAPP – Internal Medicine-Pediatrics
Read more about Rachel

“Through the development of the Lifespan Disability Clinic we have the opportunity to implement a comprehensive interprofessional model of care that I believe with have a highly positive impact on our patient’s health and function. It will also serve as a critically important training site for health professionals from many professions – both to enhance their ability to provide disability inclusive patient care as well as their ability to work effectively on an interprofessional team.”
Mary Keehn, PT, DPT, MHPE
Read more about Mary

“I completed my residency in 1990, the summer the Americans with Disabilities Act passed, with hopes that the problems of disability access, discrimination and bias would soon be a thing of the past. I was naive. Though we have made progress, there is much more work to be done. We offer these ADIH curriculum resources and invite you help advance disability-inclusive healthcare in your practice and care settings.”
Kristi L. Kirschner, MD, PM&R Physician
Read more about Kristi

“Twenty-five percent of the population identifies as having a disability so no matter what specialty a doctor chooses they need training to take proper care of people with disabilities.”
Erin Hickey, MD – Internal Medicine-Pediatrics
Read more about Erin

“I am so excited that we have created a space for openness and committed care for those who have been sidelined.”
Ann W. Jackson, PT, DPT, MPH
Read more about Ann

“This curriculum will help clinicians better understand how very difficult it is for patients, especially those with disabilities, to navigate our fragmented health care system.”
Sarah Ushkow, MSW, LCSW, CADC
The Development of the Lifespan Disability Clinic (LDC) at UIC

To address the dearth of clinical services, Dr. Caskey committed to becoming the home for a complex primary care clinic at UI-Health in the Division of Academic Medicine. She hired Erin Hickey, MD, a new Med-Peds graduate in 2020, as medical director and member of the ADIH steering committee. This team built the LDC model of care and interprofessional team. By March of 2024, with a renovated, fully accessible clinic, the Lifespan Disability Clinic (LDC) was formally launched.
The LDC offers the following services:
- Disability-inclusive Primary Care
- Coordination of medical and social care
- Management of medical supplies
- Mobility Equipment and Services
- Assistance with coordinating Transportation Services
- Referral to accessible dentistry
- Accessible clinic space
- Accessible and free parking
- Behavioral Health (with telehealth option)
- Physical and Occupational Therapy at 55th and Pulaski
- Coordination with subspecialty care (i.e., Genetics, Wound Care, Pulmonology)
- Laboratory and radiology services
- Bilingual staff (Spanish)
Photos from the ADIH Project







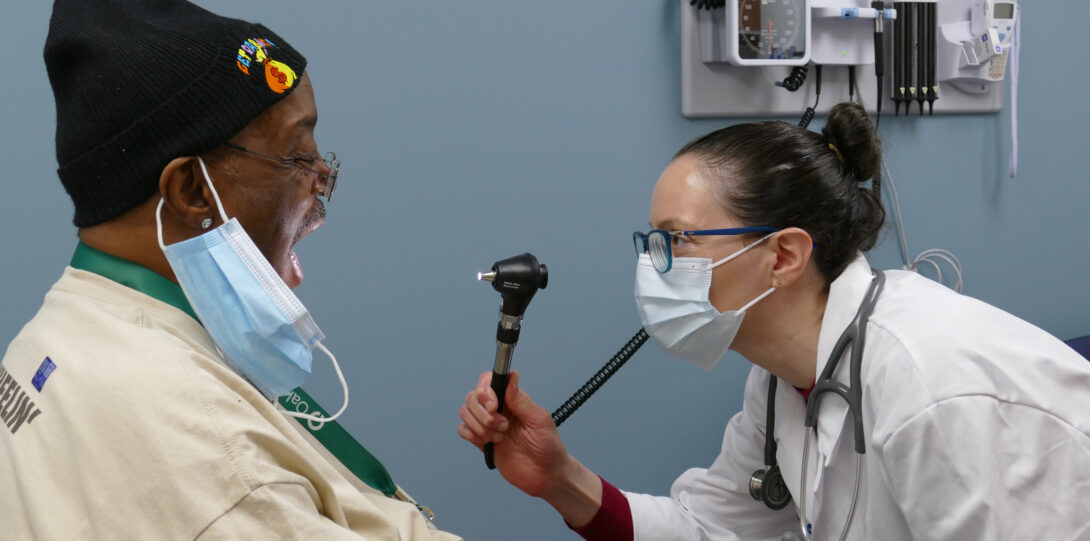


The Development of the ADIH Curriculum Project at UIC
To address the lack of healthcare professional training, the ADIH steering committee was well-positioned in 2023 to apply for the Health Resources & Services Administration (HRSA) grant, Primary Care Training & Enhancement – Language & Disability Access.
We were fortunate to be awarded support from HRSA for our project, Working to right a wrong: Training medical students to care for people with physical, intellectual and developmental disabilities (E. Hickey – Principal Investigator). As of October 2025, the award provided 100% of the total costs and totaled $2,000,000. The content are those of the authors. They may not reflect the policies of HRSA, HHS, or the U.S. Government.
Though the HRSA grant was focused on intellectual, developmental, and physical disabilities and the training of medical students, we have attempted to shape the curricula for use by all health professional learners. We will be adding new curriculum.
The HRSA Grant

HRSA is an agency of the U.S. Department of Health and Human Services; their programs provide health care to people who are geographically isolated and economically or medically vulnerable. HRSA programs also support health infrastructure through training of health professionals.
To learn more about the HRSA team, click here.
Additional Quotes

I am thrilled to see a new generation of physicians has an opportunity to learn about how to serve patients with disabilities better.
Kiyoshi Yamaki, PhD | Program Evaluator

For too long, people with disabilities have been excluded from shaping the healthcare they receive. Their engagement in training helps future clinicians see people with disabilities as people, rather than a diagnosis.
Megan Morris, PhD, MPH, CCC-SLP | Project Lead for Patient Instructor Simulated Cases
Learn about the ADIH Curriculum
The curriculum is flexible and includes modules on a variety of core topics as well as supplemental modules and individual healthcare stories of people who live with disabilities. One component of the curriculum includes an elective offered by LDC Primary Care Physicians to 4th year University of Illinois College of Medicine students called Disability Medicine.
At the conclusion of the course students will be able to:
- Provide patient-centered and disability-inclusive care to patients with a wide
range of disabilities. - Acquire a conceptual framework of disability in the context of human diversity, the lifespan, wellness, injury and social and cultural environments.
- Explore and mitigate one’s own implicit biases and avoid making assumptions
about a person’s abilities or lack of abilities and lifestyle. - Understand and identify legal requirements for providing health care in a manner
that is, at minimum, consistent with federal laws such as the Americans with
Disabilities Act (ADA), Rehabilitation Act, and Social Security Act to meet the
individual needs of people with disabilities. - Engage and collaborate with team members within and outside their own discipline to provide high quality, interprofessional team-based health care to people with disabilities.
- Collect and interpret relevant information about the health and function of patients with disabilities to engage patients in creating a plan of care that includes essential and optimal services and supports.
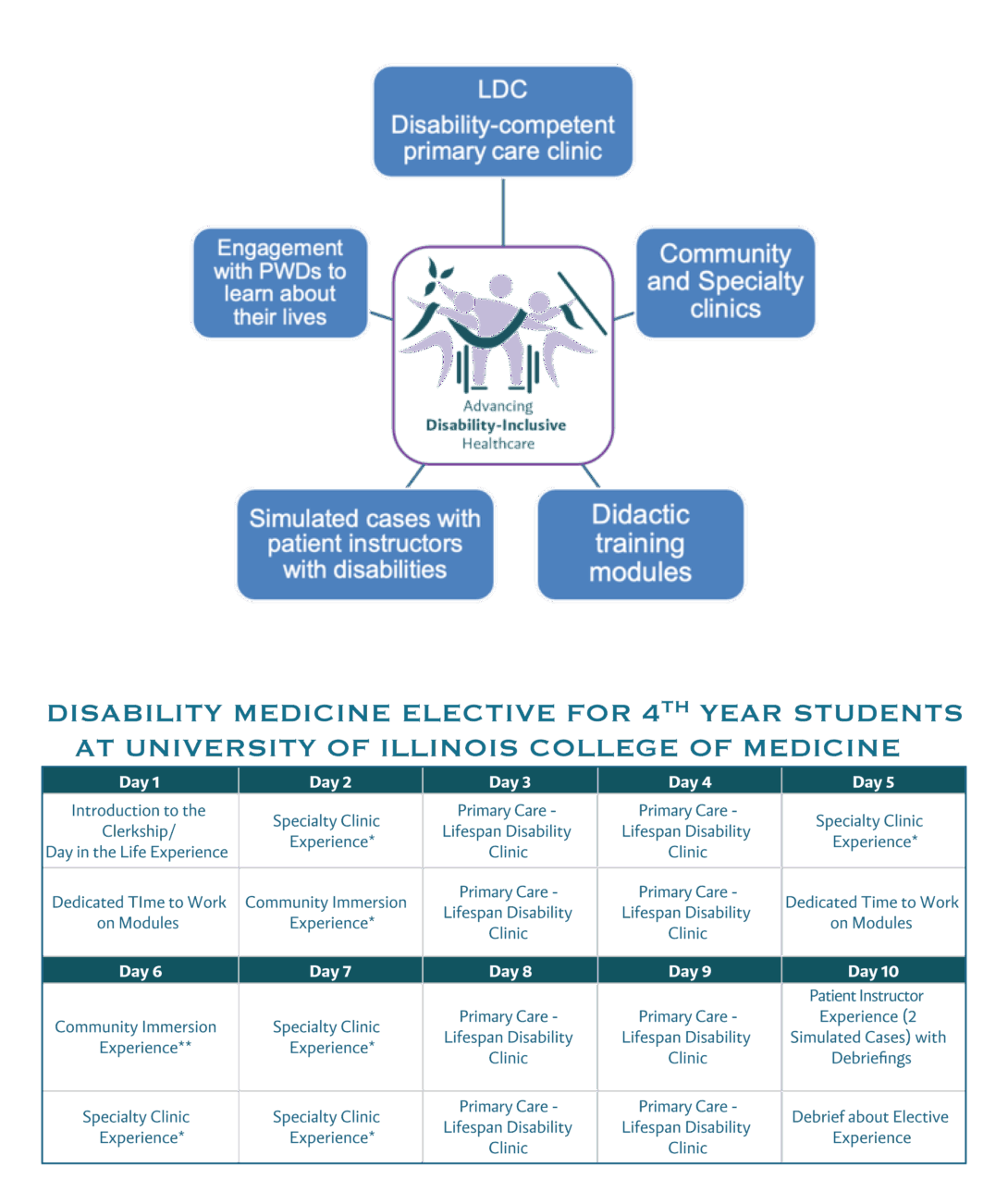
Disability Medicine Elective

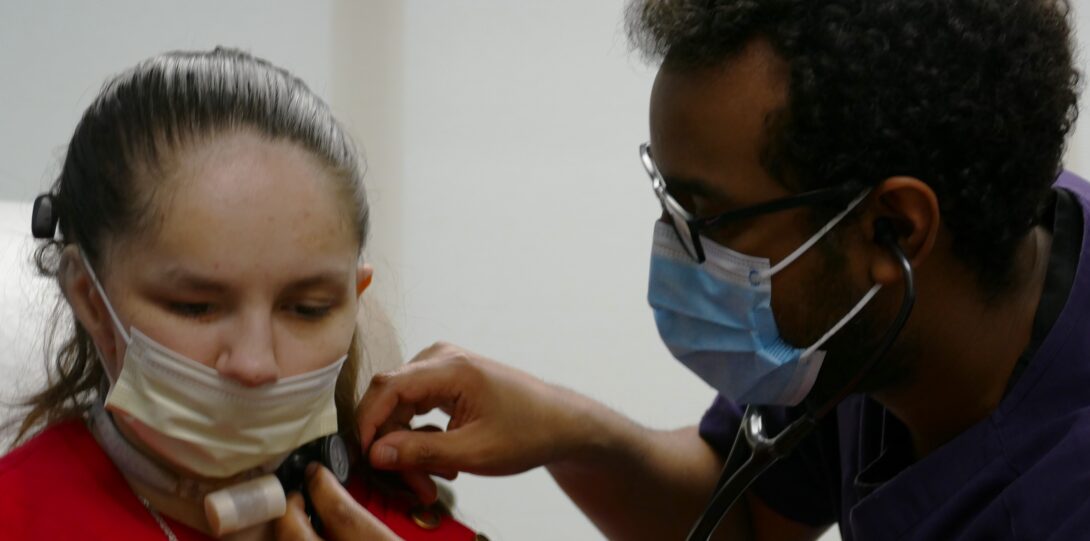
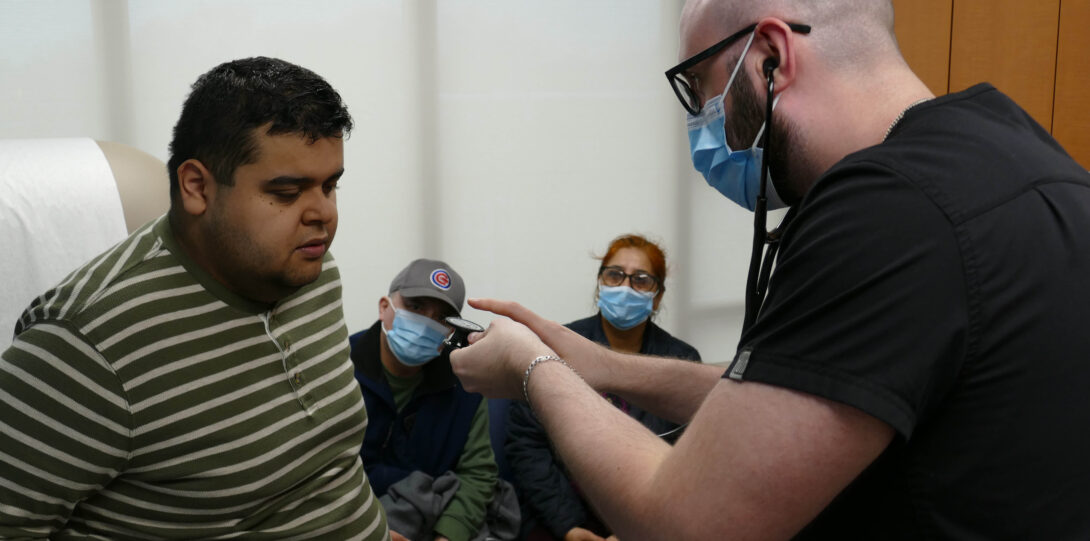
Modules

The modules are open-access, can be self-paced, and include interactive learning components. They can be done in any order or as stand alone modules.
For those looking for a basic introductory overview, you might consider Understanding Disability: Language, Identity, Culture & Models.
For a more in-depth approach, we recommend the following foundational module:
- Introduction to Disability
- A Short History of Disability Rights in the U.S.
- Legal Responsibilities of Healthcare Providers
- Michael’s Story
- Communicating with Patients with Disabilities
- Health Insurance & Other Services
Featured Stories
People with disabilities live lives as diverse as those without disabilities, yet clinicians rarely know much about the fullness of these lives. Clinicians have contact bias (seeing them only in healthcare settings when they are often sick and in need of care) and tend to focus their attention on medical diagnoses. In a society in which ableism is endemic, cultural images and stories perpetuate bias and misinformation, and clinicians receive little to no education about disability, this is a recipe for poor care. They also miss the many people with disabilities who may also be living and working side by side with you in healthcare.
We believe to mitigate these stereotypes and misinformation, we need counter-narratives, or stories about the full lives of people with disabilities that are told in partnership with them. The stories included here profile people with many disability types and health conditions, who come from diverse backgrounds and embody intersectional identities. They profile activities that give learners a window into the person’s “typical day” and often provide an intimate view of their home, school, and recreational and work environments. Some will include the voices of the person’s care partners and support systems.
We invite our learners to think of these stories not as patient stories, but simply as stories of people you may encounter in healthcare settings who happen to have disabilities. For educators who wish to use these stories in discussions or trainings we offer suggested uses and reflective questions that can be used for discussion.
We have three categories of stories: Snapshots of Community members, Leaders in the Disability Rights Movement, and Health Professionals with Disabilities.
Stay Updated with Us!
We have many more modules that will be added over time. If you wish to get updates when new materials are added, please fill out the form below.